Improving Treatment for Inflammatory Bowel Disease with Drug-Delivering Nanoparticles
[ad_1]

Drug-delivering nanoparticles could improve treatments for inflammatory bowel disease, which affects the quality of life of more than 3 million Americans, say Iowa State University researchers.
Despite current treatments, they tend to be short-term, with patients developing resistance to the drugs and relapses into inflammation and symptoms of diarrhea, severe abdominal pain, bloody stools, and extreme tiredness.
What can help?
Enter the small ball-shaped micelles.
Micelles is a self-made miracle with a diameter of only 250 billion meters. Spheres are formed when the chain of lipid molecules is exposed to water, causing the hydrophilic, water-loving heads of the molecules to form the outer shell and the hydrophobic, water-hating tails to change to the interior of the shell.
Rizia Bardhan, a professor of chemical and biological engineering at Iowa State University, and another Iowa State researcher say clever micelle designs could just be a treatment for gut conditions like Crohn’s disease and ulcerative colitis.
The US Department of Defense’s Congressional Directed Medical Research Program supports the researchers’ micellar work with a $306,000 two-year grant.
Bardhan, who has expertise in using nanoparticles for medical applications, is leading the project. Additional team members include:
- Michael Wannemuehlerwith expertise in inflammatory bowel disease, a professor of veterinary microbiology and preventive medicine
- Gregory Phillipswith expertise in the gut microbiome, is also a professor of veterinary microbiology and preventive medicine
- And Saji Ustamanwith expertise in micelle synthesis, a research scientist in chemical and biological engineering
- All affiliated with NanoVaccine Institute based in Iowa State.
Hitting Targets, Activating Gut Health
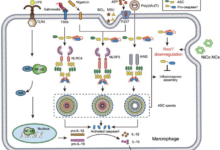
Bardhan said researchers will use hyaluronic acid, a naturally occurring biopolymer already used in human medicine, to create therapeutic micelles that can be filled with drugs that inhibit immune proteins known as STINGs. Recent studies have shown that protein activation can exacerbate inflammatory bowel disease symptoms.
The US Food and Drug Administration has not approved any drugs that block the STING protein. Researchers say this is, in part, because inhibitory drugs have been tested, but they are quickly cleared from the body and difficult to target, so they often fail to reach inflammation.
“It’s important to target drugs to the inflamed colon,Barden said. “We don’t want to accumulate nonspecifically in other organs.”
The researchers’ micelles, however, can be filled with inhibitors, keeping them in the body for hours. Hyaluronic acid also naturally targets cell receptors expressed in the inflamed colon, bringing micelles to sites of inflammation. Once there, the trigger releases a drug charge.
“The short-term impact of our project will enable the safe formulation of potent drug micelles to quickly relieve symptoms (inflammatory bowel disease) at low doses and minimal side effects, and activate a healthy intestinal environment,” according to Bardhan and Wannemuehler.
In the long term, the researchers say their STING-inhibiting micelles could impact drug delivery designs for other conditions associated with increased STING, such as Parkinson’s disease. They say the micelles can also be turned into pills for easy and convenient use.
“The biggest challenge with inflammatory bowel disease is that there is no cure.Barden said. “Many patients have become resistant to existing treatments and they don’t work anymore.”
These new, intelligently designed, purpose-built nanoparticles, say the researchers, could be the transformative agents doctors and patients are seeking.
Source: https://www.iastate.edu/
[ad_2]
Source link