Nanotechnology increases the effectiveness of T cells that attack tumors
[ad_1]
(Nanowerk News) Vanderbilt researchers are supporting the fight against cancer with technologies that increase the effectiveness of T cells that attack tumors. Cutting-edge research was recently published in the journal Immunology (“STING-activating nanoparticles normalize the vascular-immune interface to potentiate cancer immunotherapy”).
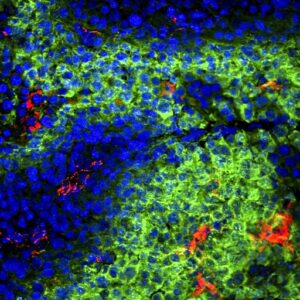
Cancers co-opt the immune and cardiovascular systems to drive their own growth, say the researchers. They do this in part by forming new blood vessels that provide essential nutrients for rapidly dividing cancer cells. T cells in the immune system also use blood vessels as conduits to find and attack tumors. But the blood vessels in tumors are often abnormal and put up barricades that block the T cells’ ability to find and kill cancer cells.
However, using nanotechnology discovered at the Immunoengineering Laboratory in Vanderbilt, researchers found that they could reverse – or normalize – defective tumor blood vessels by activating the interferon gene stimulator (STING) pathway, a component of the immune system that plays an important role in protecting against cancer. Pathogenic infections and cancer development.
John T. Wilson, professor of chemical and biomolecular engineering at Vanderbilt and corresponding author on the paper, said the technology’s ability to reprogram tumor blood vessels could help make T cells more effective at killing cancer cells.
“This allows T cells to better infiltrate and destroy tumors in mouse models of kidney and breast cancer and increases the efficacy of immunotherapies currently used in patients,” said Wilson, who is also the Principal Investigator of the Immunoengineering Lab and Chancellor of the Faculty of Associates.
In the publication, the researchers also discuss testing their STING-activating nanoparticle (STAN) technology in surgically removed tumors from patients with renal cell carcinoma (RCC). Consistent with findings from their experiments with mice, they found that STAN “exhibits superior immunostimulatory activity,” offering “preliminary evidence supporting the potential use of STAN as a strategy to coordinate antitumor innate immunity and vascular remodeling in human RCC.”
Such a breakthrough is urgently needed. This year, nearly two million new cancer cases and more than 600,000 cancer deaths are projected in the United States, according to the American Cancer Society.
“While this technology is not yet ready for use in cancer patients, our study reveals an exciting new strategy for enhancing response to cancer immunotherapy,” said Wilson.
[ad_2]
Source link