Potential Treatment for Glioblastoma Using Nanoparticles
[ad_1]
A new nanoparticle treatment for glioblastoma has been developed by Northwestern Medicine researchers, according to research published in Nature Communications.

Maciej Lesniak, MD, chair and Michael J. Marchese Professor of Neurosurgery, is the senior author of the study published in Nature Communications. Image Credit: Northwestern University
Glioblastoma is one of the most complex and common types of primary brain cancer, which is a lethal and treatment-resistant cancer, according to the National Brain Tumor Society. Over several years, the five-year survival rate for glioblastoma patients has approached 7% and has remained unchanged.
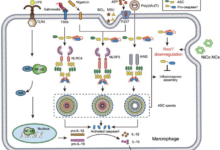
Previous Northwestern Medicine research has revealed that glioblastoma tumors add to large numbers of tumor-associated myeloid cells immunosuppressive (TAMC), impairing the immune system’s ability to fight tumors and minimizing the efficacy of chemotherapy and radiation.
Immunosuppression is a hallmark of the tumor microenvironment. TAMC is a key driver of immunosuppression and therapy resistance. Because TAMC makes up 30 to 50 percent of brain tumor mass, there is an urgent need to develop new therapeutic strategies to target and modulate these immunosuppressive cells in brain tumors..
Peng Zhang, Ph.D., First Study Author and Assistant Professor, Neurosurgery, Northwestern University
In the existing study, the researchers focused on TAMC cultured with nanoparticles they built to offer the dimeric amidobenzimidazole, or diABZI, a newly developed synthetic compound, targeting a protein called interferon gene stimulator, or STING. Also, the nanoparticles were loaded with antibodies targeting CD47 and PD-L1, which are two immune checkpoint proteins that are overexpressed in TAMC and glioblastoma tumors after radiotherapy.
According to studies, TAMCs that received therapy produced significantly less immunosuppressive proteins and augmented immunostimulatory proteins.
When the nanoparticles were used to treat mice with glioblastoma, the researchers saw a spike in the number of activated T-cells, which are normally responsible for boosting the immune response against tumors but are generally lacking in brain tumors. As per the study, treated mouse T cells infiltrated the tumor in larger numbers and extended the life cycle of the mice.
In about 70% of animals, tumors are eradicated following nanoparticle treatment and radiation therapy, which are the standard treatment for glioblastoma.
Addressing tumor immunosuppression is key to designing effective immunotherapeutic strategies. This approach paves the way to modulate the tumor microenvironment in such a way as to enhance immunotherapeutic potential.
Maciej Lesniak, MD, Author and Senior Study Chair and Michael J. Marchese Professor, Neurosurgery, Northwestern University
Then, the researchers replicated the experiment using blood and tumor samples from glioblastoma patients and again observed reprogrammed TAMC and activated anti-tumor T cells.
The findings suggest that nanoparticle therapy could be a successful way to complement existing treatments and amplify the immune response in glioblastoma, said Lesniak.
Lesniak, Zhang, and their co-workers are confident of bringing nanoparticle therapy to clinical trials, said Zhang.
We also wanted to gain more insight into how the host immune response might contribute to the therapeutic efficacy or therapeutic resistance of these tumors. We also wanted to incorporate immune metabolism and bioinformatics into our multi-disciplinary research so that we could do a thorough job of designing next-generation therapies against brain tumors..
Peng Zhang, Ph.D., First Study Author and Assistant Professor, Neurosurgery, Northwestern University
Lesniak and Zhang are members of the Robert H. Lurie Comprehensive Cancer Center at Northwestern University.
This study was funded by National Institutes of Health/National Cancer Institute grant R37CA266487 and Northwestern Brain Tumor SPORE P50CA221747.
Journal Reference
Zhang, P. et al. (2019). Targeted tumor-associated myeloid cell therapy synergizes with radiation therapy for glioblastoma Proceedings of the United States National Academy of Sciences. https://doi.org/10.1073/pnas.1906346116
Source: https://www.northwestern.edu/
[ad_2]
Source link